A Layered Approach to Indoor Air Quality

The past 2.5 years of the COVID pandemic have put a big spotlight on indoor air quality and the spread of infectious disease. I’ve been writing about various aspects of indoor air quality since I started this blog in 2010, so a lot of this wasn’t new to me. Still, I’ve learned some new things, had others reinforced, and generally feel like I have a more complete view of the subject than I did before 2020. Here’s my big picture view of IAQ now along with an example of how it was put into action at a conference I attended last month.
Good IAQ advice
1. COVID is airborne. If you’re still wiping down groceries, washing your hands obsessively, or hiding behind plexiglass, you’re not doing the most effective things to prevent COVID or other infectious diseases. Some people call those things hygiene theater. The problem is mainly particles that float in the air for hours (aerosols), not droplets that fall quickly.
2. The best method to avoid COVID is to stay away from people who have it. That’s source control. The COVID protocols that relied on testing were based on this method. You test positive; you can’t get in.
3. If someone with COVID is in a room with you but they’re wearing an effective mask (KN95 or N95 worn properly), that’s source control and filtration.

4. If you filter the air with MERV-13 filters or better to remove particulate matter, your exposure is reduced if someone is in the room with COVID and not wearing a mask.
5. By bringing clean outdoor air into a building and mixing it with indoor air, you’re diluting any pollutants in the indoor air. That’s ventilation.
6. Ultraviolet germicidal irradiation (UVGI) is another proven air-cleaning method. But the key is that they must be properly engineered. If not, they may be ineffective or even destructive. To deactivate viruses in the air stream with an in-duct UV lamp, the power level has to be high enough for the air flow rate. And if the UV hits vulnerable materials, as is the case with some filters, it can damage them. This technology is best in hospitals and other buildings with a lot of people.
7. Carbon dioxide can be an effective way to monitor how much dilution is happening with ventilation air. With masks and good filtration of the indoor air, however, you can have high CO2 levels and little spread of infectious disease. Monitoring CO2 is only one part of getting clean indoor air.
8. Additive air cleaners may not make the air any cleaner. They may also do harm. There are no standards governing how they’re tested except for ozone emission. It’s best to avoid them.
9. Control the humidity. Neither too high nor too low is good. We’ve known for a long time that humidity affects indoor air quality. Now Stephanie H Taylor, MD and some others say that keeping the relative humidity between 40 and 60 percent can reduce the spread of infectious disease. There’s still some debate about that, though. (See this paper from the journal Nature.) One thing to be aware of with keeping the relative humidity higher is that you have to have a building enclosure that can take it in a cold climate. Otherwise, you can rot a building and even destroy it, as they did at Harvard.
An example from a conference
At the 2022 Westford Symposium on Building Science, also known as Building Science Summer Camp, we had a three day conference with about 400 people. Three of the four sessions on the first day were on the topic of indoor air quality and the spread of infectious disease, including my presentation on the Corsi-Rosenthal DIY box fan air cleaner. And we practiced what we preached.

Professor Bill Bahnfleth spoke on buildings and infection control (pdf) and evaluated the layered approach to IAQ at the event. It included:
- Upgrading the filtration in the room to MERV-13
- Increasing the mechanical ventilation with outdoor air
- Using three Corsi-Rosenthal boxes
- Irradiating the air with four upper-room ultraviolet germicidal irradiation lamps (one shown above)
- Some people (I was one) wearing masks
Below is the slide showing Bahnfleth’s calculation of the exposure reduction due to this layered approach.
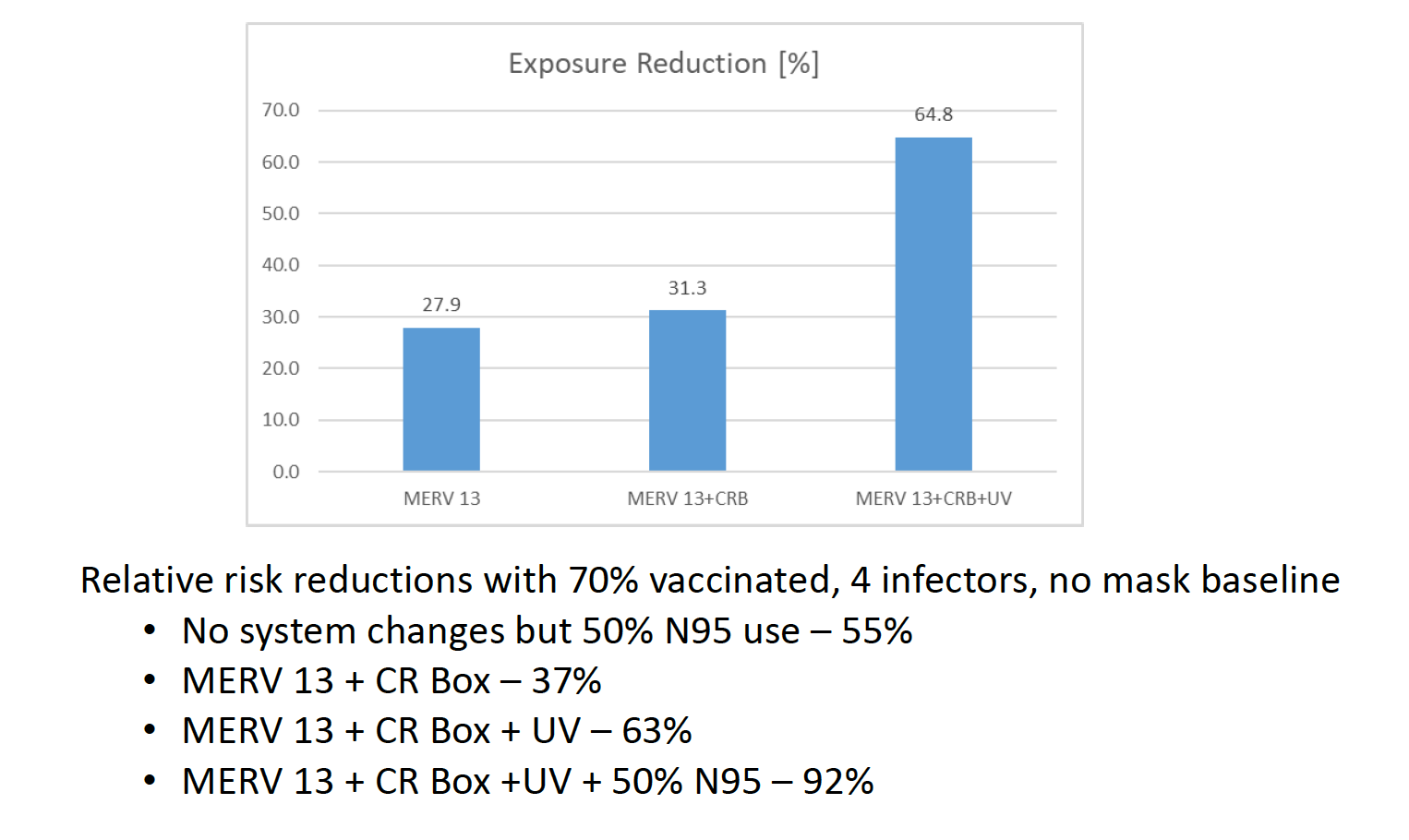
Based on his calculations, we had an overall exposure reduction in the conference room of about 63%. If half the people in the room had been wearing masks, it would have been over 90%. The actual mask-wearing rate was less than 20%.
Of course, this is one example and incomplete anecdotal evidence, but there’s only one case of someone getting COVID at the conference. He’s pretty sure he got it there, but not in the main conference room. He was in a meeting in a small room that didn’t have those protective measures mentioned above. It’s possible more people got it and didn’t report back, but one out of about 400 people is pretty good.
The bottom line is that the workhorses of good indoor air quality are source control, filtration, ventilation, and humidity control. Ultraviolet germicidal irradiation is appropriate in some settings but must be engineered properly.
Allison A. Bailes III, PhD is a speaker, writer, building science consultant, and the founder of Energy Vanguard in Decatur, Georgia. He has a doctorate in physics and writes the Energy Vanguard Blog. He also has written a book on building science. You can follow him on Twitter at @EnergyVanguard.
Related Articles
Carbon Dioxide and the Air You Rebreathe
2 Reasons to Avoid Most Electronic Air Cleaners
3 Ways to Get Cleaner Indoor Air With Filtration
DIY Box Fan Air Cleaner Update
Comments are moderated. Your comment will not appear below until approved.
This Post Has 9 Comments
Comments are closed.

It remains a mystery to me how even folks with our advanced scientific knowledge have such a low mask adoption.
Finally, approaching IAQ in the home!
I believe the HVAC and IAQ should be part of every system, at least sealing all duct work guided by static pressure tests, then treating g the air to be cleaner. All homes have different needs but the common denominator is the Health of the Occupant. For a $600.00 investment I built a system with a MERV 13, 5 inch Filter, with a UV Lighting, and also used and “Air Cycler” control using the fan motor of my Furnace to pull air thru my filter on every 1/2 hour, a 3 hour Cycle (During Cleaning of the Home), and a 24 Cycle for High Pollen or outdoor air quality issues that might be introduced to the home or if we are sick.
Our Family has reduced sickness and I believe the cost saving in Pharmaceuticals and Doctors Visits have been dramatically reduced thru the use of this system.
I Inspect homes from 1898 to present, all could use this type of system properly sized to support the Occupants of their Homes.
Please God don’t let the residential code people see this.
So for high performance new residential construction would you say that MERV-13 on both HVAC and ERV systems is good protection without the need for a dedicated separate whole house filtration system (higher than MERV-13)?
As Allison has pointed out in several other posts in the past, simply installing a MERV-13 filter into an existing system or in a new HVAC or ERV installation is likely to create pressure-drop issues at the filter. We bought our 1987 home in 2013 and immediately installed a new HVAC system to replace the existing failed unit, but the new system uses the existing return and supply ductwork, etc. The return filters are at the entry points for the main (low-level) return and smaller high-level return (rather than at the air handler, which is attic mounted). I jacked up the MERV rating using what were thought to be good-quality 1-inch pleated filters, confident that I would be improving everything. The filters were sucked into the returns by about 1.5 inches, but they showed the expected collection of dirt and dust on them. Then I read Allison’s article describing the effect of pressure drop at the returns on overall system flow, which is something I had been concerned about since I could not get enough supply flow to evenly heat and cool certain rooms in the house. These 1-inch thick filters were providing very high pressure drops because they were trying to stop small particles (the high MERV), so even with the support network of the frame they still were being sucked into the openings due to the resistance. A few months ago I switched to Honeywell 4-inch deep filters that mount in the normal 1-inch frames (and stick out the back, where there has always been plenty of space in our case), which retain the high MERV ratings (in the 13-14 range) but the deep pleats allow the air to flow with very low pressure drop, close to a low MERV pleated filter. The air flow through the returns and out of the supply ducts immediately increased. Voila, the supply issue had disappeared. So, be sure to take the pressure drop on your filter choice(s) into account, and keep it as low as possible to maintain your system supply sufficiency.
Could you share more info on this Honeywell filter that mounts are inch filter to a 1 inch opening? My search didn’t turn one up.
The Honeywell filters are about 3 to 4 inches deep, but they have frames that mount in conventional 1-inch deep holders, as long as there is sufficient room behind the filter holder to allow for the depth of the filter plus several inches for air transport. In our case, we have two returns, one that was built into a space adjacent to a closet, so the behind-frame space is about 1 foot; the other was built with a deep box metal inlet going to a 12-inch duct, which is 8-10 inches deep. Both provide adequate space for air flow with no significant restrictions. In addition to Honeywell, there are knock-off brands that offer similar deep pleated and low-pressure-drop pleated filters, but I cannot speak for their quality or effectiveness. The ones that we got fit our particular filter sizes. Looking at the actual filters, I see that I was mistaken about the MERV level, which is MERV 10. The ones we got are the current 3-inch deep filters rather than 4-inches deep (which the original products were), but they are described as having the same MERV value and pressure drop as the previous versions (likely by changing the details of the filter fabric, so that the more-shallow installation would fit more situations). The filters that I purchased do not display the model number, but you should be able to find these or equivalent products being sold. We bought our genuine Honeywell filters through an on-line HVAC supply company called SupplyHouse.com. The 24×24 version went by the SKU FC40R1078 on their web site, where the “40” is actually a carry-over from Honeywell’s original product that was 4″ deep; the ones we got, and the ones you are likely to get, are actually 3″ deep.
As a home designer/ planner who is very interested in IAQ, I’ve been thinking of a simplified way to reduce the chances of disease at home without making the home much more expensive. The HVAC system could have a fresh air supply running through a filter, dehumidifier, and UV before being mixed into the return air duct. This could increase the air pressure. The laundry/ mud room could be easily sanitized and have a fan for air exhaust. A person could enter from the garage, put their clothes in the wash, take a shower, and put on clean clothes. The exhaust would maintain a lower air pressure in this room, reducing contaminants from getting into the rest of the house. Also, an exhaust could be added to bedrooms for someone that is sick. A variable speed fan could raise the volume of air into the air return to compensate for how many exhaust fans are running. (This system would allow a kitchen range hood to operate more effectively).
Member of Team Airborne here! Thanks for advocating all the right things. I swear to God, I’m tired of hearing local HVAC companies pushing ionizers.
Anyways, I’ll also plug my own little part here. If you carry a CO2 meter around, I’d love it if you share your data with my crowdsourced co2 tracking project, CO2 trackers!
https://www.co2trackers.com/home
Dr. Kashif Pirzada runs a similar and slicker project, The Raven Clean Air app, but mine was first! 😉🤣